Understanding what is narcolepsy is the first step to managing it. This neurological condition causes overwhelming daytime sleepiness and other distinct narcolepsy symptoms. Fortunately, effective narcolepsy treatment options exist, combining lifestyle changes with medication to improve quality of life and help regain control over your days.
At its core, the answer to what is narcolepsy involves the brain’s inability to regulate sleep-wake cycles normally. It is not simply feeling tired. It is a chronic neurological condition characterized by sudden, uncontrollable attacks of sleep. People with this condition can fall asleep during any activity, at any time of day, which poses significant challenges to daily life.
This condition is fundamentally a sleep disorder. However, it’s rooted in the brain’s chemistry. Scientists believe that most cases of narcolepsy with cataplexy are caused by a deficiency in a chemical neurotransmitter called hypocretin (also known as orexin). This chemical helps sustain alertness and regulate the sleep-wake cycle. Without it, the brain cannot properly control when you are awake or asleep.
The investigation into what is narcolepsy has led to the classification of two main types. Type 1 narcolepsy includes a symptom called cataplexy, which is a sudden loss of muscle tone triggered by strong emotions. People with Type 1 have low levels of hypocretin. Type 2 narcolepsy does not involve cataplexy, and individuals usually have normal levels of hypocretin.
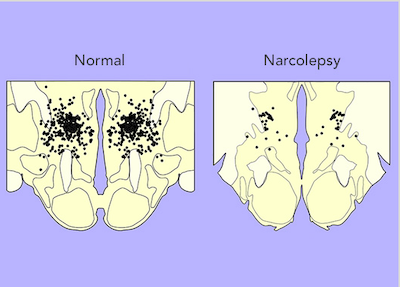
(Credit: Harvard Medical School)
It is important to view this as a legitimate medical condition. The term disease narcolepsy helps frame it correctly, moving away from misconceptions of laziness or poor lifestyle choices. Recognizing it as a disease narcolepsy is crucial for seeking and receiving appropriate medical support. Living with this condition means committing to careful, lifelong management strategies. Understanding the fundamentals of what is narcolepsy empowers patients and their families.
Living with this condition means navigating a world that often misunderstands the profound need for sleep. The journey begins with identifying the signs. The core experience is not just tiredness; it is a persistent and overwhelming sleepiness that does not go away with rest. This is a key part of understanding what is narcolepsy.
What are the most common narcolepsy symptoms to look for?
The range of narcolepsy symptoms can vary greatly from person to person. However, some classic signs are central to a diagnosis. The most universal symptom is excessive daytime sleepiness (EDS). This is the hallmark of the condition. It manifests as a constant feeling of fogginess and an irresistible urge to sleep, often leading to involuntary sleep episodes or “sleep attacks.”

These sleep attacks can last from a few seconds to several minutes. They can happen in the middle of a conversation, while eating, or even while driving. This makes EDS one of the most disruptive and dangerous narcolepsy symptoms. It interferes with work, school, relationships, and the simple ability to stay present and engaged in life.
Cataplexy is another of the most specific symptoms of narcolepsy, almost exclusively found in Type 1. It is a sudden, brief loss of voluntary muscle control. This is typically triggered by strong emotions like laughter, excitement, surprise, or anger. An episode can be mild, like a drooping of the eyelids, or severe, causing a complete collapse of the body while the person remains fully conscious.

(Credit: The New England Journal of Medicine)
Sleep paralysis is another frightening experience for many. It is a temporary inability to move or speak that occurs just as you are falling asleep or waking up. The episode is brief, but it can feel terrifying. The mind is awake, but the body remains temporarily paralyzed, which is one of the more unsettling symptoms of narcolepsy.
Many people also experience vivid and often bizarre dreams or hallucinations. When these occur while falling asleep, they are called hypnagogic hallucinations. When they happen upon waking, they are known as hypnopompic hallucinations. These are not just regular dreams; they feel incredibly real and can be frightening. These are key narcolepsy symptoms.
Finally, disrupted nighttime sleep is a common yet paradoxical symptom. While a person with narcolepsy is excessively sleepy during the day, they may struggle to stay asleep at night. They might wake up frequently, leading to a fragmented and unrefreshing night’s sleep. These combined narcolepsy symptoms create a complex challenge for those affected.
Exploring modern narcolepsy treatment approaches
There is no cure for narcolepsy, but a comprehensive narcolepsy treatment plan can significantly improve symptoms and quality of life. Management is not just about medication. It involves a combination of behavioral strategies, lifestyle adjustments, and support from healthcare providers, family, and friends. A good plan is always personalized.
One of the most effective behavioral strategies is scheduling short, regular naps. Planned naps of about 20 minutes at strategic times during the day can help manage excessive daytime sleepiness. For many, this simple routine provides a few hours of renewed alertness. This is a foundational part of any effective narcolepsy treatment.

Maintaining a strict sleep schedule is also vital. Going to bed and waking up at the same time every day, even on weekends, helps regulate the body’s internal clock. This practice, known as good sleep hygiene, can improve the quality of nighttime sleep. It strengthens the sleep-wake cycle, which is a core goal of narcolepsy treatment.
Lifestyle adjustments play a significant role. Regular exercise, particularly aerobic activity, can promote better alertness during the day and deeper sleep at night. However, it is important to avoid exercising too close to bedtime. A balanced diet is also crucial. Heavy meals and sugary foods can increase sleepiness, while smaller, more frequent meals can help maintain energy levels.
Avoiding alcohol, nicotine, and caffeine is also a recommended part of narcolepsy treatment. While caffeine may seem like a good idea for staying awake, it can disrupt nighttime sleep and lead to a worse cycle of sleepiness. Alcohol and nicotine can also interfere with sleep quality. These substances can make the primary narcolepsy symptoms much worse.
Support systems are an often-underestimated part of narcolepsy treatment. Connecting with others who understand the condition can reduce feelings of isolation. Support groups, counseling, and educating friends and employers can create a more accommodating environment. A holistic narcolepsy treatment plan addresses both the physical symptoms and the emotional impact of the disorder.

Understanding your narcolepsy medication options
For most individuals, lifestyle changes alone are not enough. Narcolepsy medication is often a necessary component of the treatment plan to manage the most disruptive symptoms. The specific medications prescribed depend on the individual’s unique set of symptoms. A specialist will work with the patient to find the right regimen.
To combat excessive daytime sleepiness, stimulants are a common form of narcolepsy medication. Medications like modafinil or armodafinil are often the first choice. They promote wakefulness with a lower risk of addiction and side effects compared to older stimulants. Traditional stimulants like methylphenidate may also be used. This is a core part of narcolepsy treatment.
:max_bytes(150000):strip_icc()/hivtreatment-GettyImages-1268333171-aac755dd53b8455bae86ca3a571a3ed1.jpg)
For controlling cataplexy, as well as sleep paralysis and hallucinations, other types of narcolepsy medication are used. Antidepressants, such as selective serotonin reuptake inhibitors (SSRIs) and serotonin and norepinephrine reuptake inhibitors (SNRIs), can help manage these REM-sleep-related symptoms. They work by suppressing the stage of sleep where these symptoms arise.
A powerful and unique narcolepsy medication is sodium oxybate. It is taken at night in two doses and is highly effective at improving fragmented nighttime sleep. As a result, it can significantly reduce both excessive daytime sleepiness and cataplexy. It is a cornerstone of modern narcolepsy treatment for many patients with Type 1.
The process of finding the right narcolepsy medication can involve some trial and error. It is essential to maintain open communication with your doctor about how you are feeling and any side effects you experience. Over time, your doctor might need to fine-tune the prescribed dosages. The goal is to find a balance that maximizes symptom control while minimizing adverse effects.
Ultimately, managing narcolepsy is a collaborative effort between the patient and their healthcare team. While the question of what is narcolepsy points to a complex neurological issue, the path forward is clear. A combination of lifestyle strategies and carefully selected narcolepsy medication allows many to lead full, productive, and engaging lives. The journey to managing this disease narcolepsy is one of hope and empowerment.
- WEBSITE Wikipedia Authors. (n.d.). Narcolepsy. Wikipedia English. [Article Link]
- WEBSITE Harvard Medical School Team. (2022, April 13). The science of narcolepsy. Harvard Medical School. [Article Link]
APA 7: TWs Editor. (2025, September 24). What is Narcolepsy: A Deep Dive into the Sleep Condition. PerEXP Teamworks. [Article Link]

















