Type 1 diabetes is an autoimmune condition where the body stops producing insulin. Knowing the type 1 diabetes symptoms is key for early action. The type 1 vs type 2 diabetes comparison shows critical differences. Proper type 1 diabetes treatment is essential for managing the condition and living a healthy, full life.
What causes type 1 diabetes and is it genetic?
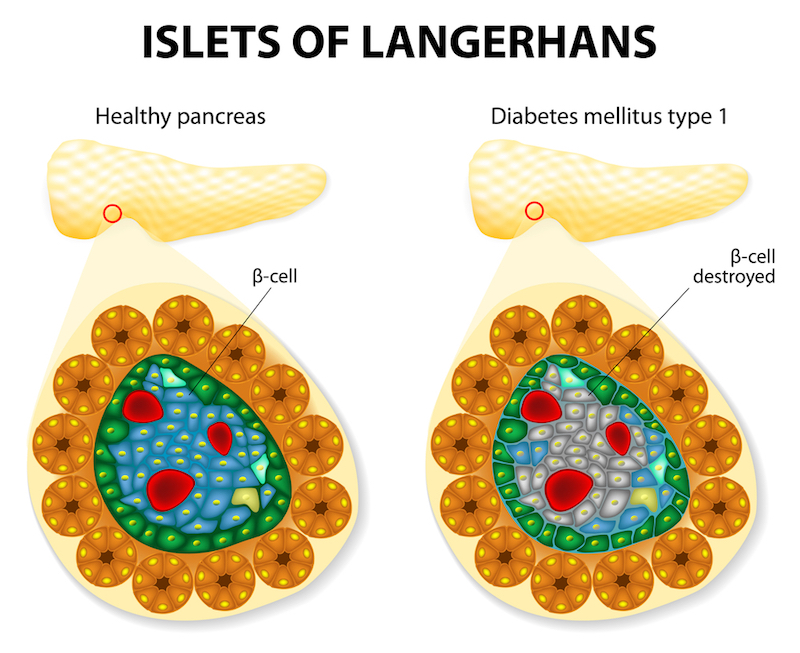
Type 1 diabetes occurs because of a malfunction in the body’s immune system. The immune system incorrectly flags the pancreas’s insulin-producing cells as hostile threats. These cells, called beta cells, are then attacked and destroyed. Without beta cells, the body can no longer produce insulin, a hormone vital for regulating blood sugar.
This autoimmune attack is the direct cause of the condition. Insulin acts like a key. It unlocks your body’s cells to let glucose (sugar) enter and be used for energy. When there’s no insulin, glucose builds up in the bloodstream. This leads to high blood sugar levels, which cause the many health problems associated with diabetes and type 1.
Many people ask if the condition is purely genetic. Genetics do play a significant role. Certain genes, particularly those known as HLA genes, can make a person more susceptible to developing type 1 diabetes. Having these genes doesn’t guarantee you will get the disease. It only increases your risk factor.
Think of it as having a genetic predisposition. The genes load the gun, but an environmental factor often pulls the trigger. The exact triggers are not fully understood. However, researchers believe certain viruses or even components of our diet might initiate the autoimmune response in genetically vulnerable individuals.
So, while there is a clear genetic link, the condition results from an intricate interaction between genetic factors and environmental influences. A parent with the disease may have a child who never develops it. Conversely, the vast majority of people diagnosed have no direct family history.
Diabetes and type 1 can begin to develop regardless of a person’s age. It is most commonly diagnosed in children, adolescents, and young adults. However, it is possible to be diagnosed later in life. This is sometimes referred to as latent autoimmune diabetes in adults (LADA), but the underlying cause remains the same autoimmune process.
Understanding what causes this disorder helps demystify it. Consuming excess sugar or making certain lifestyle choices are not the causes of this condition. It is an autoimmune condition where the body’s defense system turns on itself. This fundamental point is crucial for both patients and the public to grasp. Research continues to explore the precise triggers to one day prevent this autoimmune disease.
The primary type 1 diabetes symptoms and signs to identify
Recognizing the type 1 diabetes symptoms early is extremely important. An accumulation of glucose in the blood happens when the body is unable to produce insulin. Subsequently, the body attempts to flush out the surplus sugar via urination. This process triggers a cascade of clear and often sudden warning signs. Prompt diagnosis can prevent serious complications.
The most common type 1 diabetes symptoms are often called the “4 Ts.” These are Thirst (polydipsia), Toilet (polyuria), Tiredness (fatigue), and Thinner (unexplained weight loss). A person may experience intense thirst that seems unquenchable. This is because the body is pulling fluid from tissues to flush out the excess sugar.

This leads directly to frequent urination, including waking up multiple times at night. Because the body is losing so much fluid, dehydration is a risk. All these processes are exhausting for the body, causing profound fatigue. The body feels drained of energy because it cannot use its main fuel source, glucose, effectively.
Unexplained weight loss is another key indicator among the type 1 diabetes symptoms and signs. Without insulin, the body’s cells are starved for energy. To compensate, the body starts breaking down fat and muscle tissue for fuel. This results in weight loss even if the person is eating normally or more than usual.
Beyond the 4 Ts, other type 1 diabetes symptoms can appear. Blurred vision is a common complaint. High blood sugar levels can pull fluid from the lenses of the eyes, affecting their ability to focus. This issue often resolves once blood sugar levels are brought under control.
Other type 1 diabetes symptoms and signs include frequent infections, such as skin or yeast infections, and slow-healing sores. Elevated blood glucose levels can weaken the immune system’s effectiveness against bacteria and viruses. It can also affect circulation, making it harder for the body to heal itself.
If these type 1 diabetes symptoms are ignored, a life-threatening condition called diabetic ketoacidosis (DKA) can develop. This occurs when the body, desperate for energy, breaks down fat at such a high rate that it produces ketones. Because ketones have acidic properties, they can create a toxic state in the body. DKA requires immediate medical attention.
Type 1 vs type 2 diabetes: what’s the key difference?
Understanding the type 1 vs type 2 diabetes comparison is essential because they are fundamentally different conditions. While both result in high blood sugar, their causes, onset, and management approaches vary significantly. Confusing the two can lead to misconceptions about why a person has diabetes and how it should be treated.
The primary difference between type 1 and type 2 diabetes lies in their origin. As discussed, type 1 diabetes is an autoimmune disease where the body destroys its insulin-producing cells. Therefore, the body produces very little or no insulin. It is an issue of insulin absence.

In contrast, the defining characteristic of type 2 diabetes is primarily insulin resistance. Although the pancreas continues to produce insulin, the body’s cells are unable to use it efficiently. Eventually, the pancreas might struggle to meet the body’s elevated need for insulin, leading to a decline in its production.
Another point in the type 1 vs type 2 diabetes debate is the typical age of onset. The former is often diagnosed in childhood or young adulthood, though it can occur at any age. The condition typically appears suddenly, and its symptoms are often intense. Type 2 diabetes typically develops more slowly over many years and is more common in adults over 45.
Lifestyle factors play a different role in the type 1 vs type 2 diabetes discussion. This autoimmune disorder is not caused by diet or lifestyle. Type 2 diabetes, however, is strongly linked to factors like obesity, physical inactivity, and diet, alongside a strong genetic predisposition.
This leads to another key difference between type 1 and type 2 diabetes: treatment. Everyone diagnosed must take insulin to survive. They need to replace the hormone their body can no longer make. This is non-negotiable from the moment of diagnosis.
For type 2 diabetes, treatment often begins with lifestyle changes like diet and exercise. Oral medications may be prescribed to help the body use insulin more effectively or to produce more of it. While some people with type 2 diabetes may eventually need insulin, it is not always the first line of treatment. The core of the type 1 vs type 2 diabetes distinction is simple: one is an autoimmune disease, the other is a metabolic disorder.
A guide to effective type 1 diabetes treatment and management
Effective type 1 diabetes treatment is not a one-size-fits-all plan. It is a dynamic and personalized strategy that requires daily attention. Managing the condition aims to maintain blood sugar readings inside a specific, healthy range. This helps a person feel healthy and prevents long-term complications through a careful balance of insulin, diet, and physical activity.
Insulin therapy is the fundamental basis for the treatment of type 1 diabetes. Since the body cannot produce its own insulin, it must be administered externally. This is typically done through multiple daily injections with an insulin pen or syringe. A small device called an insulin pump works by supplying a steady, non-stop stream of insulin.
A crucial part of the treatment of type 1 diabetes involves regular blood sugar monitoring. This gives the person and their healthcare team the data needed to make adjustments to insulin doses. This can be done with a finger-prick blood glucose meter or a continuous glucose monitor (CGM). A CGM uses a sensor placed under the skin to track glucose levels 24/7.
Nutrition is another vital component of a good management plan. It is not about a restrictive diet. Instead, it focuses on understanding how different foods affect blood sugar levels. Learning to count carbohydrates is a critical skill that enables someone to precisely align their insulin dosage with the food they consume.
Regular physical activity is also highly encouraged as part of the treatment of type 1 diabetes. Exercise helps the body use insulin more efficiently and has numerous health benefits. However, it also impacts blood sugar levels, so it is important to learn how to manage glucose before, during, and after being active to avoid low blood sugar (hypoglycemia).
Living with this condition is a constant learning process. The type 1 diabetes treatment plan will likely change over time due to factors like age, lifestyle changes and new technologies. Working closely with a healthcare team is key to successful long-term management of diabetes and type 1.
The daily demands of this treatment plan can be challenging. It requires diligence and patience. However, with the right tools, knowledge, and support, people with type 1 diabetes can manage their condition effectively and lead long, healthy, and active lives without limitations.
Can type 1 diabetes be cured permanently?
This is a question filled with hope for millions of people. Currently, type 1 diabetes does not have a permanent cure. The autoimmune process that causes the condition cannot be reversed with current medical technology. Once the beta cells are destroyed, they do not grow back. The focus of care remains on lifelong management, not a cure.
However, the landscape of type 1 diabetes treatment is advancing rapidly. Research is exploring several exciting avenues that could one day lead to a cure or, at the very least, a life free from daily insulin injections and blood sugar checks. These strategies aim to either replace the lost beta cells or stop the autoimmune attack.

One area of research involves the transplantation of a pancreas or its specific islet cells. This can restore natural insulin production, but it has major drawbacks. The procedure is complex, and the person must take powerful immunosuppressant drugs for life to prevent their body from rejecting the transplant.
A more advanced approach is the development of an “artificial pancreas.” These are also known as closed-loop systems. They connect a CGM to an insulin pump via a smart algorithm. The system automatically adjusts insulin delivery based on real-time glucose readings, mimicking the function of a healthy pancreas. This is a powerful form of treatment of type 1 diabetes that greatly reduces the daily burden of management.
Perhaps the most promising research focuses on immunotherapy. Researchers are investigating methods to re-educate the immune system, preventing its assault on beta cells. If this could be done at the time of diagnosis, it could preserve any remaining insulin-producing cells. This would make managing the condition significantly easier.
So, while a permanent cure for the disease remains in the future, the outlook is incredibly hopeful. The progress in technology and medical research has transformed how the condition is managed. The goal is to make living with diabetes and type 1 safer, easier, and less intrusive, bringing us closer to a world without the daily challenges of this disease.
- WEBSITE Nemours KidsHealth Team. (n.d.). What is Type 1 diabetes? Nemours KidsHealth. [Article Link]
- WEBSITE Department of Health & Human Services. (n.d.). Diabetes type 1. Better Health Channel. [Article Link]
- JOURNAL Holt, R. I., DeVries, J. H., Hess-Fischl, A., Hirsch, I. B., Kirkman, M. S., Klupa, T., Ludwig, B., Nørgaard, K., Pettus, J., Renard, E., Skyler, J. S., Snoek, F. J., Weinstock, R. S., & Peters, A. L. (2021). The management of Type 1 diabetes in adults. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care, 44(11), 2589–2625. [Article Link]
- JOURNAL Hirsch, I. B., Juneja, R., Beals, J. M., Antalis, C. J., & Wright, E. E. (2020). The Evolution of Insulin and How it Informs Therapy and Treatment Choices. Endocrine Reviews, 41(5), 733–755. [Article Link]
APA 7: TWs Editor. (2025, September 10). Type 1 Diabetes: A Guide to Its Causes, Symptoms, and Care. PerEXP Teamworks. [Article Link]